Complete.MD Web Portal and Client Release 03-06-2026
BUGS
CPT to DX Code Error
Resolved an issue where DX codes could not be correctly associated to CPT codes with modifiers, causing false validation errors even when selections were saved properly. The CPT search logic now accounts for modifiers and unique CPT identifiers, ensuring DX codes are assigned to the correct CPT entries.
ERA Search Amount
Fixed an issue in ERA Search where entering decimal values in the Amount filter caused errors. The Amount filter now properly supports two-decimal currency values.

FEATURES
PA Warning Flag
Portal
- Added a Requires Prior Authorization toggle in the Payer Plan modal.
- Added support for configuring Warning Days for expiring prior authorizations in the Payer Plan modal.
- Added an alert in the Claim Ticket pop-out, within the Prior Authorization section, to notify staff when a claim is being created for a patient whose payer plan requires prior authorization.


Client
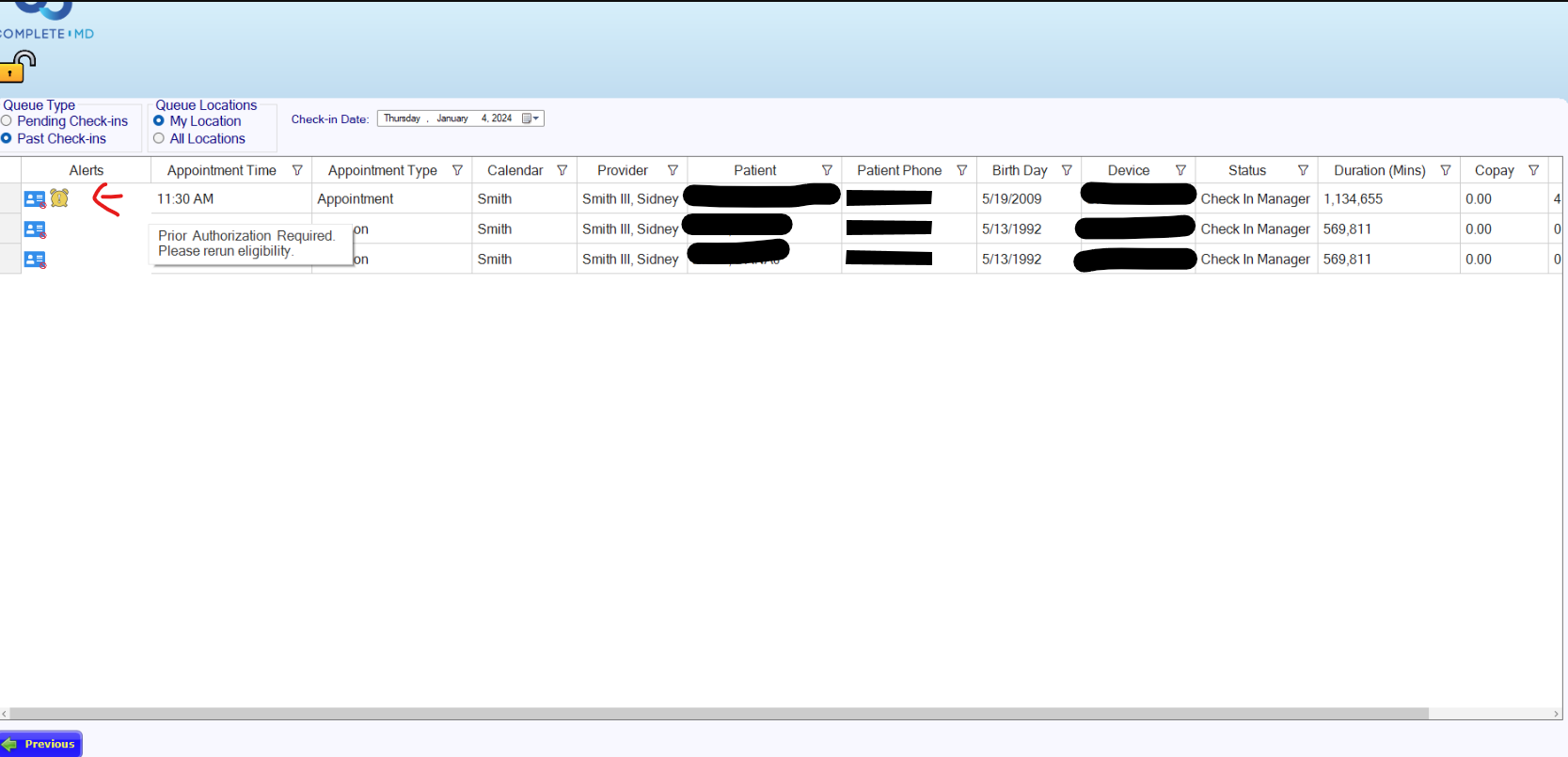
- Added an alert in Checkout Manager to notify staff when a scheduled patient’s payer plan requires prior authorization.
-
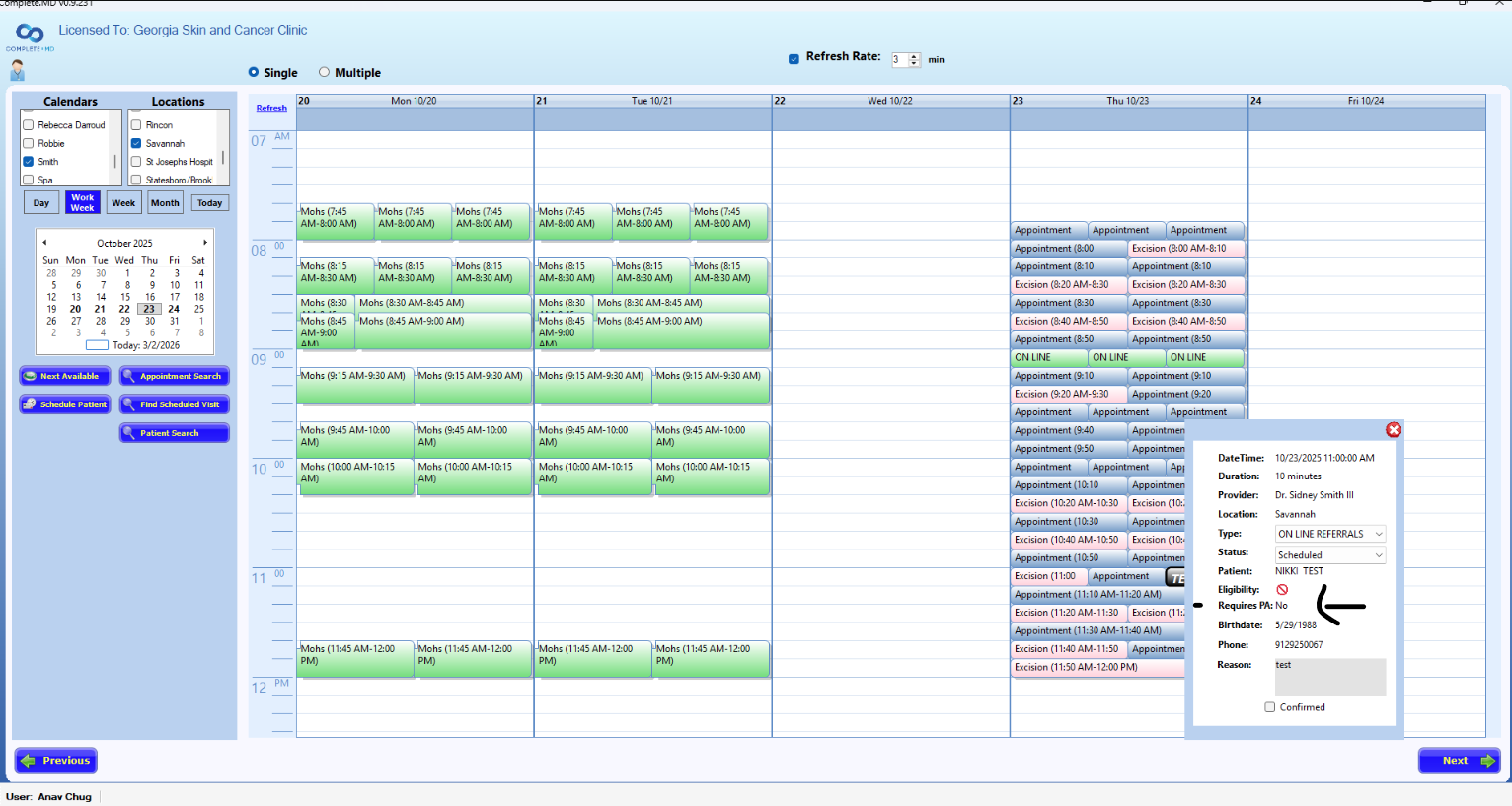
Added a Requires PA indicator in the Scheduler module, within the Appointment Details popup below Eligibility, displaying Yes/No based on whether the patient’s payer plan requires prior authorization.
Delete Payers and Payer Plans
Added the ability for administrators to delete payers and payer plans, allowing organizations to clean up outdated billing data and improve coordination between front registration and the billing department.


ERA Search Excel Report
Added an Export button to the ERA Search page, enabling users to export search results to Excel for easier review and reporting.



